Contents
You wake at 3am and your mind is already switched on.
Your eyes are open, but your body feels like it’s running away with itself, playing back events, financial pressures, conversations, emails and disagreements, over and over.
Your mind jumps ahead to worst-case outcomes – “I’m going to lose respect”, “I’ve let someone down”, “I’m not enough”.
What felt manageable at 2pm feels catastrophic at 3am.
Your chest is tight before the day has even started. Your stomach feels hollow. Your jaw is already clenched.
You tell yourself to calm down, and you try to talk yourself out of it:
- “It’s nothing.”
- “Stop overthinking.”
- “Just go back to sleep.”
But the more you push it away, the louder it seems.
Frankly, it can feel frightening – alien, unfamiliar, and difficult to understand. When something feels that overwhelming, the instinct is often to escape it.
But instead of running from it, the more useful move is to understand it.:
“What is happening to me?”
“Why does it feel physical?”
“Why can’t I switch it off?”
“Is this a sign I’m not coping?”
“Is something wrong with me?”
Before anything else, understand this – anxiety is not weakness, there isn’t anything wrong with you, and the interplay between anxiety and stress is normal to most people at some point, or even multiple points, in their lives. You might see it as a sign that you’re not coping, but anxiety is often evidence that you are coping. It means your system is trying to protect you. It means you care about the outcome. It means something matters.
Anxiety is not the absence of strength. It is your nervous system mobilising to deal with something it perceives as important.
Anxiety is your physical alarm system trying to protect you from danger (LeDoux, 2012). Cortisol naturally brings you out of slumber early in the morning. It happens earlier at the moment, waking you up at 3am rather than 5am or 6am because your cortisol levels are raised due to stress response brought on by anxiety (Chrousos, 2009; McEwen, 2007).
Men and women often interpret anxiety and stress through different internal lenses.
For many men, anxiety can represent a perceived threat to their ability to provide, protect and fix, roles that have frequently been central to their sense of identity (you can read more about that here. The link opens in a new tab). If strength has been equated with steadiness and control, then feeling vulnerable to anxiety may be experienced as evidence that those roles are compromised. In that context, anxiety is not simply an uncomfortable emotion but a challenge to self-concept, which can, in some cases, contribute to anger, defensiveness, emotional withdrawal or, over time, the development of compulsive coping behaviours (Addis & Mahalik, 2003).
Anxiety can present differently in women, where it is often characterised by rumination and repetitive, future-oriented thinking that centres on perceived personal shortcomings. The internal narrative may shift toward self-evaluation — “what is wrong with me?” — reflecting a tendency toward self-critical processing rather than outward expression (Nolen-Hoeksema et al., 2008). Whereas some men may experience anxiety as a threat to their role in relation to others, what it means about their capacity to provide, protect or perform, many women are more likely to internalise the distress, interpreting it as evidence of personal inadequacy.
When you experience anxiety, your brain believes you are in danger. Its priority is to get you to safety, and that requires speed. To achieve that, it triggers fear, anger or urgency so that you act quickly – whether that means crossing the road to avoid a group that feels threatening, or bracing yourself to confront something. This is not weakness; it is your biological survival system doing exactly what it was designed to do.
At the same time, heightened stress reduces your ability to think clearly. Some people struggle to find words, feel mentally foggy or blocked, or notice their mind going blank. This happens because the brain shifts resources away from higher cognitive functions and toward survival processes (Arnsten, 2009). It is a normal response.
What often makes anxiety more frightening is the physical intensity that follows. Once the psychological alarm sounds, the body responds with a racing heart, shallow breathing and tightness in the chest (McEwen, 2007; Goldstein, 2010). The sensations feel real because they are real.
For some, the fear is not only the anxiety itself but the thought, “What if this is something worse, like a heart attack?” The physical overlap can feel alarming (American Heart Association, 2023). Understanding this distinction is important, because while the sensations are powerful, they are usually the body’s stress response — not a sign that you are about to die.
With that understanding in place, we can begin to look at what to do next.
What is Anxiety and Stress?

Many of the clients I work with aren’t entirely sure what anxiety and stress actually are. The words get used interchangeably because advice online can be contradictory, and before long, people are trying to fight something they don’t fully understand.
Most people don’t really get it at all. That’s because we don’t take the time to absorb what anxiety and stress are. We’re taught to get on with things, to fulfil our role in life, and to keep moving. This doesn’t leave much space for pausing and asking, “What am I actually feeling?”
That’s not your fault. That perception to get on with it is shaped by the messages you absorbed growing up. Maybe you heard, “Just get on with it.” Maybe you heard, “Be kind. Don’t be difficult.” Those messages shaped how you now respond to distress. Some people learn to push it down and carry on. Others turn it inward and question themselves.
In both cases, anxiety is there, but it is the script around it that you’ve been taught through the course of your life that determines how you handle and deal with it.
It matters that we get this right because when we fail to see the relationship between anxiety and stress clearly, we stop seeing it as an alarm system, and we begin instead to fear the experience of anxiety itself. That can lead to panic attack when we try to suppress it, override it, or power through it. In doing so, we often prolong the very thing we are trying to escape.
Panic attacks are frightening because the physical sensations – chest tightness, a racing heart and shortness of breath – can resemble symptoms associated with a heart attack. While panic attacks themselves are not fatal, the intensity of the experience can make it feel dangerous. A panic attack reflects a surge in the body’s alarm system, often signalling that anxiety has reached a level that can no longer be ignored.
In simple terms, anxiety is the perception of danger, or the early warning system. Your body and mind register that something feels unsafe around you. The threat may not be concrete or visible, but it feels real enough to create unease. There is a tightening, a scanning, and a sense that something requires attention. Panic attack is that alarm system going off louder.
Stress is the mobilisation that follows, the need to do something. Once danger is perceived, the body prepares for action. Heart rate rises. Muscles tense. Attention narrows. You feel energised, braced, ready to respond. You don’t know what it is cognitively but you’ve got an urge to do something – to fight, run away and so forth.
When people say, “I feel stressed,” they are usually describing the physical side of that preparation – tension in the chest, the shallow breathing, the irritability of not understanding what is going on and “why now”. What often goes unnoticed is that it began with anxiety, a perceived threat, sometimes subtle, sometimes barely conscious.
If we don’t recognise this sequence, we risk dismissing stress as something we can simply endure or drive through. It is true that acute stress responses can settle within minutes once the threat passes because the system is designed to surge and then stand down. But the difficulty comes when we repeatedly enter that state without realising it because it has become second nature to dismiss it and move on, or to blame ourselves for how we feel. Living in and out of activation, hoping it will just disappear, is what becomes chronic stress. And chronic stress does not simply stay in the mind. It affects the cardiovascular system, immune function, sleep quality and cognitive clarity. The body was built for short bursts of mobilisation. It was not built for sustained anticipation of danger.
Anxiety and stress are not design flaws. They have a purpose. So rather than ignoring them or battling against them, it is more useful to ask:
- “What am I perceiving as dangerous right now?”
- “Where did that perception come from?”
- “What is this response trying to protect?”
When we understand the origin and function of the signal, we stop treating it as the enemy. We begin working with it instead of against it, and it will settle down as we tune into it.
Anxiety is Evolutionary
For most of human history, anxiety had a clear purpose because it gave humans an advantage over predators. If a tiger stepped out of the trees, the body needed to react instantly so heart rate surged, muscles tightened, and attention narrowed. Humans either ran or fought, and once the danger passed, the system settled down. Early humans understood anxiety because they could perceive it with the senses so the stress response was short, sharp and survival-focused (McEwen, 2007; LeDoux, 2012).
Today, the tiger rarely has stripes. Instead it may be a difficult conversation, an uncertain income, a relationship that feels fragile, something on social media, or a fear of humiliation or failure. Remember the thoughts racing through your mind when anxiety happens? These are your tigers and they’re roaming around in your mind.
Those threats that cause anxiety don’t have to be in the wild do the body to react in the same way. The “threat” is often psychological these days, symbolic or anticipated. The tiger lives in thought. However, your nervous system cannot easily distinguish between immediate physical danger and vividly imagined social risk. So it prepares you anyway (LeDoux, 2012; Brosschot et al., 2006).
The response still makes sense biologically. It’s just firing in a world very different from the one it evolved for (McEwen, 2007).
Why Understanding Comes First

If you only try to “calm down” without understanding what is causing it, your system can interpret that as suppression.
What it responds to more reliably is safety. So before we look at deeper patterns, we stabilise the body, not to eliminate anxiety but to signal that the threat has passed, that the body can calm down (Thayer & Lane, 2000) and we can look at what it was and why it happened.
Below are practical ways to do that.
What Actually Works
All of these will feel counterintuitive when you’re in anxiety but they do work and can work very well if you use them at the first signs of feeling threat.
Box Breathing
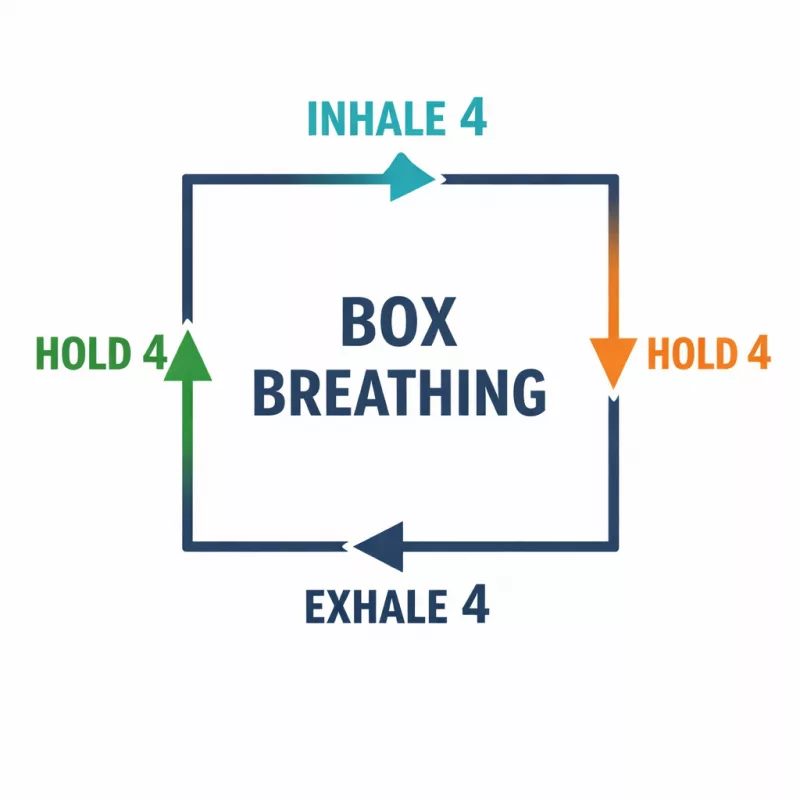
Breathe in for 4 seconds.
Hold for 4 seconds.
Exhale for 4 seconds.
Hold for 4 seconds.
Repeat for two minutes.
Box breathing works because slow, rhythmic breathing under your control stimulates the Parasympathetic Nervous System (the calming system), particularly via the vagus nerve.
The extended rhythm reduces sympathetic activation (fight–flight) and signals to the brain that the environment is stable (Grossman & Taylor, 2007; Thayer & Lane, 2000). It is about signalling safety to your body so within 2 minutes you will feel much better.
This strategy can also build into a longer term breathing exercise that can top up your calming system so when you need the resources to deal with anxiety and stress, they’re already there to bring them under your control more quickly. As you get to the bottom of the exhale, notice the peace, quietness that exists in the space between ending the breath and starting the next one.
Tense and Release
This is actually called Progressive Muscle Relaxation but feels counterintuitive because what I am asking of you here, is the tensing of all muscle groups at the same time. Tense every muscle in your body firmly for 5–7 seconds when you feel anxiety taking hold. You might feel tense already but over exaggerating it really helps.
Don’t hold your breath!
Hold the tenseness like a board, hold it and then release immediately – don’t hold back, literally let the tenseness fall away.
Notice the contrast – this is important to notice that you’re okay, nothing happened. You can relax and be safe. Repeat this as many times as you need but most clients find that twice is enough.
Anxiety often involves unconscious muscular bracing. When you deliberately tense and release, you:
- Increase awareness of where you are holding stress
- Interrupt chronic contraction
- Provide the nervous system with a “discharge” of activation
Progressive muscle relaxation has been shown to reduce physiological arousal and sympathetic activation (Conrad & Roth, 2007).
The rapid release phase sends feedback to the brain that the body is no longer preparing for impact.
It is a physical reset. Don’t stop there. What you can now do is engage the thinking brain. This works well with this technique to allow you to feel under control again.
Engage the Thinking Brain
When anxiety spikes, the limbic system (emotional threat detection) dominates. The prefrontal cortex, which is responsible for reasoning and regulation, becomes less active (Arnsten, 2009).
One way to counter this is deliberate cognitive engagement.
- Do a Wordle.
- Count backwards in 7s from 300.
- Do mental arithmetic.
- Spell a long word backwards.
This is not distraction in the avoidant sense. It is neural rebalancing and will help to bring you back to a state or ‘normality’ for you. You will feel like you’re fighting yourself initially which why it pairs with the previous technique well but keep going, engage the brain.
If you can’t count back in 7s, that is okay, count forward in twos and then make it slightly harder as you notice it becomes easier.
You are recruiting the prefrontal cortex, which helps modulate limbic over-activation. The brain cannot fully sustain threat mode while simultaneously performing structured cognitive tasks.
You are reminding the system: we are thinking, not surviving.
Why These Techniques Are Not the Whole Story

These tools stabilise the system. They reduce intensity. They prevent escalation. But they do not answer the deeper question:
“Why is my system activating this strongly in the first place?”
They won’t fix anxiety or stress because the reason they happen is because you are programmed to ignore it, or perhaps you know what is causing it but can’t face it, or maybe you have no idea at all and it is simply a battle of survival.
Anxiety often protects identity. It guards against humiliation, abandonment, loss of control or failure (Gilbert, 2010).
For many men, strength and composure become armour (Addis & Mahalik, 2003). For many women, relational sensitivity becomes hyper-responsibility, which can increase vulnerability to rumination (Nolen-Hoeksema et al., 2008).
Anxiety is often the emotional echo of these collisions.
Moving Beyond Coping
Coping tools reduce intensity. Understanding reduces recurrence.
Chronic stress becomes harmful when activation is prolonged rather than resolved (McEwen, 2007; Brosschot et al., 2006). So, when you explore:
- What your anxiety is trying to prevent
- What it fears would happen if you relaxed
- Where you learned that you must always be strong, pleasing or prepared
… you regain choice and control.
The same system that once created chronic tension can be redeployed into discernment and grounded self-trust. You stop living in anticipation of threat. You begin responding instead of reacting. If you are living with ongoing stress or anxiety, know this:
It makes sense.
Your task is not to shame it away. Your task is to understand it.
If you would like to work through your anxiety properly – not just manage symptoms, but understand what is driving them – I offer person-centred counselling grounded in psychological depth and safety. We begin by stabilising the stress response using techniques like those above. Then we look carefully at the patterns beneath it, so you are no longer bracing for impact in your own life.
You do not need a diagnosis. You do not need to have the words yet.
If this resonates, you can get in touch here, or arrange an initial conversation here.
Awareness first. From there, things begin to shift.
Sources
American Psychological Association. (2023). Stress effects on the body. https://www.apa.org/topics/stress/body
Arnsten, A. F. T. (2009). Stress signalling pathways that impair prefrontal cortex structure and function. Nature Reviews Neuroscience, 10(6), 410–422. https://doi.org/10.1038/nrn2648
Brosschot, J. F., Gerin, W., & Thayer, J. F. (2006). The perseverative cognition hypothesis: A review of worry, prolonged stress-related physiological activation, and health. Journal of Psychosomatic Research, 60(2), 113–124. https://doi.org/10.1016/j.jpsychores.2005.06.074
Chrousos, G. P. (2009). Stress and disorders of the stress system. Nature Reviews Endocrinology, 5(7), 374–381. https://doi.org/10.1038/nrendo.2009.106
Dedovic, K., Duchesne, A., Andrews, J., Engert, V., & Pruessner, J. C. (2009). The brain and the stress axis: The neural correlates of cortisol regulation in response to stress. NeuroImage, 47(3), 864–871. https://doi.org/10.1016/j.neuroimage.2009.05.074
Goldstein, D. S. (2010). Adrenal responses to stress. Cellular and Molecular Neurobiology, 30(8), 1433–1440. https://doi.org/10.1007/s10571-010-9606-9
Grossman, P., & Taylor, E. W. (2007). Toward understanding respiratory sinus arrhythmia: Relations to cardiac vagal tone, evolution and biobehavioral functions. Biological Psychology, 74(2), 263–285. https://doi.org/10.1016/j.biopsycho.2005.11.014
LeDoux, J. E. (2012). Rethinking the emotional brain. Neuron, 73(4), 653–676. https://doi.org/10.1016/j.neuron.2012.02.004
McEwen, B. S. (2007). Physiology and neurobiology of stress and adaptation: Central role of the brain. Physiological Reviews, 87(3), 873–904. https://doi.org/10.1152/physrev.00041.2006
Nolen-Hoeksema, S. (2001). Gender differences in depression. Current Directions in Psychological Science, 10(5), 173–176. https://doi.org/10.1111/1467-8721.00142
Nolen-Hoeksema, S., Wisco, B. E., & Lyubomirsky, S. (2008). Rethinking rumination. Perspectives on Psychological Science, 3(5), 400–424. https://doi.org/10.1111/j.1745-6924.2008.00088.x
Thayer, J. F., & Lane, R. D. (2000). A model of neurovisceral integration in emotion regulation and dysregulation. Journal of Affective Disorders, 61(3), 201–216. https://doi.org/10.1016/S0165-0327(00)00338-4
van der Kolk, B. A. (2014). The body keeps the score. Viking.
Brosschot, J. F., Gerin, W., & Thayer, J. F. (2006). The perseverative cognition hypothesis. Journal of Psychosomatic Research, 60(2), 113–124. https://doi.org/10.1016/j.jpsychores.2005.06.074
Conrad, A., & Roth, W. T. (2007). Muscle relaxation therapy for anxiety disorders. Journal of Anxiety Disorders, 21(3), 243–264. https://doi.org/10.1016/j.janxdis.2006.04.001
Gilbert, P. (2010). The compassionate mind. Constable & Robinson.
Johnson, S. M. (2008). Hold me tight. Little, Brown.


